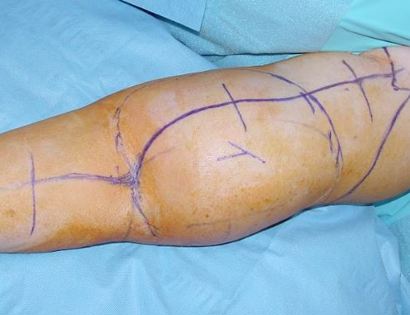
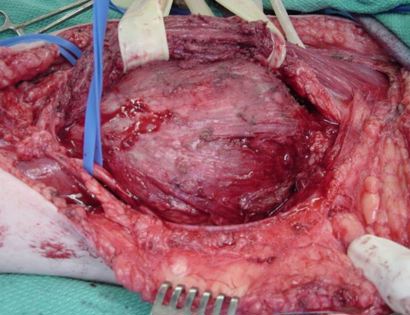
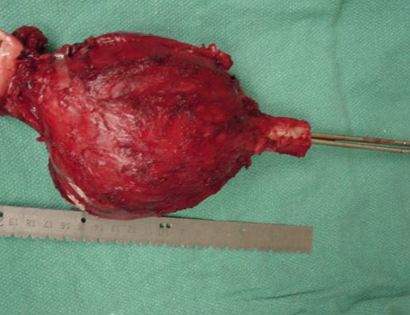
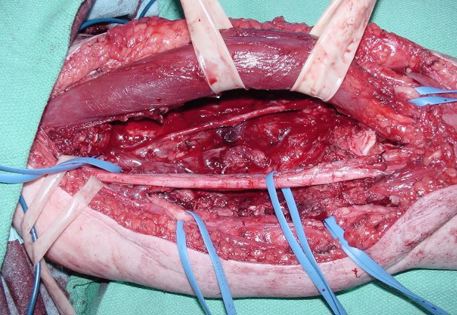
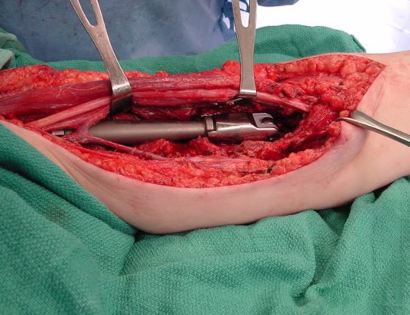
What is a limb-sparing surgery of the lower arm/elbow?
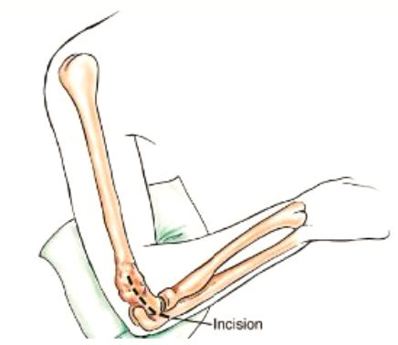
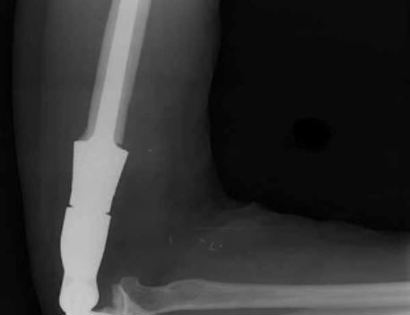
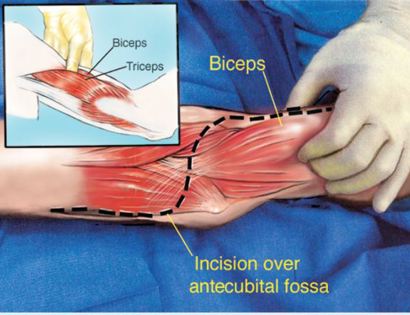
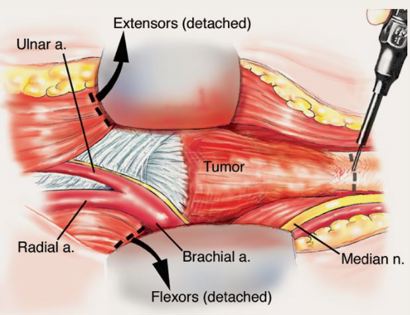
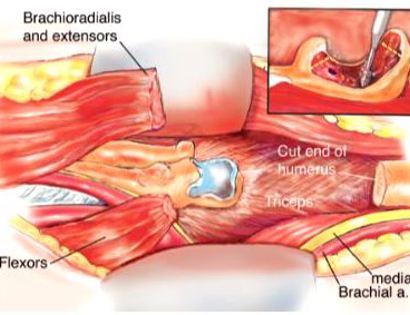
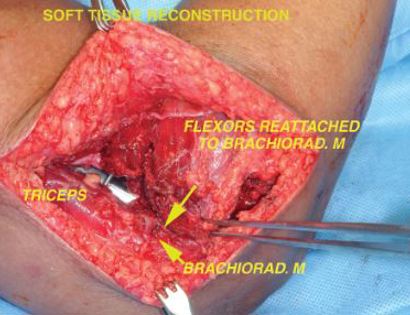
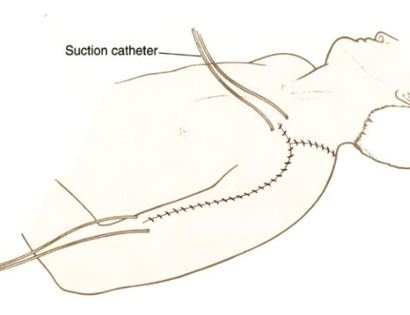
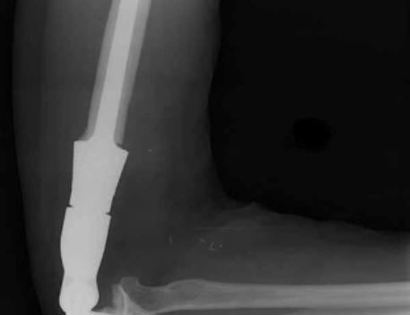
The elbow consists of your humerus, ulna, and radius bone. The distal (lower part) humerus is a relatively rare site for primary bone sarcomas and accounts for approximately 1% of all bone tumors. It is more commonly involved by neoplasm (tumor) through metastatic disease. The distal humerus or elbow joint also can be secondarily involved by soft tissue sarcomas arising from the adjacent muscles and soft tissues including undifferentiated pleomorphic sarcoma. Limb-sparing surgery can be performed for approximately 95% of tumors arising from the lower humerus. In some instances, the extremity cannot be saved and an amputation is performed.
Contraindications for saving the limb may include neurovascular invasion, infection, pathological fracture, extensive disease, contamination from a poorly performed biopsy, recurrent disease.