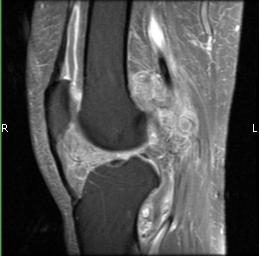
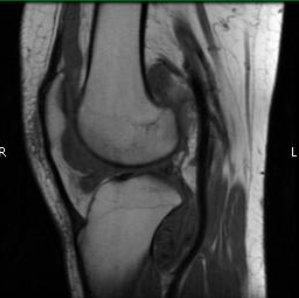
Pigmented Villonodular Synovitis (PVNS)
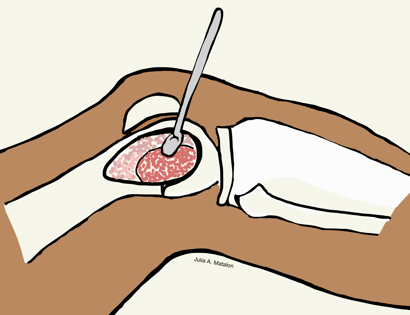
Pigmented Villonodular Synovitis (PVNS) is a benign (non-cancerous) condition that occurs due to overgrowth of the synovium, the tissues that line the joints, or production of excess synovial fluid. A majority of PVNS cases occur in the knee. Treatment of PVNS commonly includes a synovectomy to remove the excess tissue and fluid.